Periodontics is the branch of dentistry devoted to this foundation, focusing on the prevention and treatment of gum disease and the preservation of oral health. It begins with a clear definition of periodontics as a specialty, extends into its critical importance for both dental and systemic well-being, and emphasizes how gum disease prevention protects against serious conditions such as heart disease, diabetes, and imbalances in the body’s microbiome.
The field addresses the most common periodontal diseases and conditions, from early gingivitis to advanced periodontitis, along with issues such as gum recession and bone loss. To understand how treatment works, it is necessary to explore the periodontal anatomy and structures, including the periodontal ligament, alveolar bone, and gingival, that form the essential support system for teeth and implants.
Treatment solutions in periodontics are wide-ranging, including non-surgical scaling and root planing, surgical approaches such as gum reshaping, regenerative therapies like bone grafting, and implant procedures that depend on healthy periodontal tissues. The specialty gains definition when compared with others, showing the differences between periodontics, orthodontics, and endodontics, as well as the distinction between the role of a general dentist and a periodontist.
Recognizing when specialized care is necessary is vital for long-term health. Periodontics outlines the signs that indicate professional intervention is required, from bleeding gums and loose teeth to persistent halitosis and pre-implant assessments, ensuring the foundation of the smile remains strong throughout life.
What Is Periodontics?
Periodontics is a specialized branch of dentistry that focuses on the prevention, diagnosis, and treatment of diseases affecting the gums and the supporting structures of the teeth. It also involves the placement of dental implants and the treatment of oral inflammation. The structures that periodontics is concerned with are collectively known as the periodontium, which includes the gums, periodontal ligament, and the jawbone.
A dentist who specializes in this field is called a periodontist. They complete an additional two to three years of focused training beyond dental school to become experts in gum disease, complex gum surgeries, and dental implant placement.
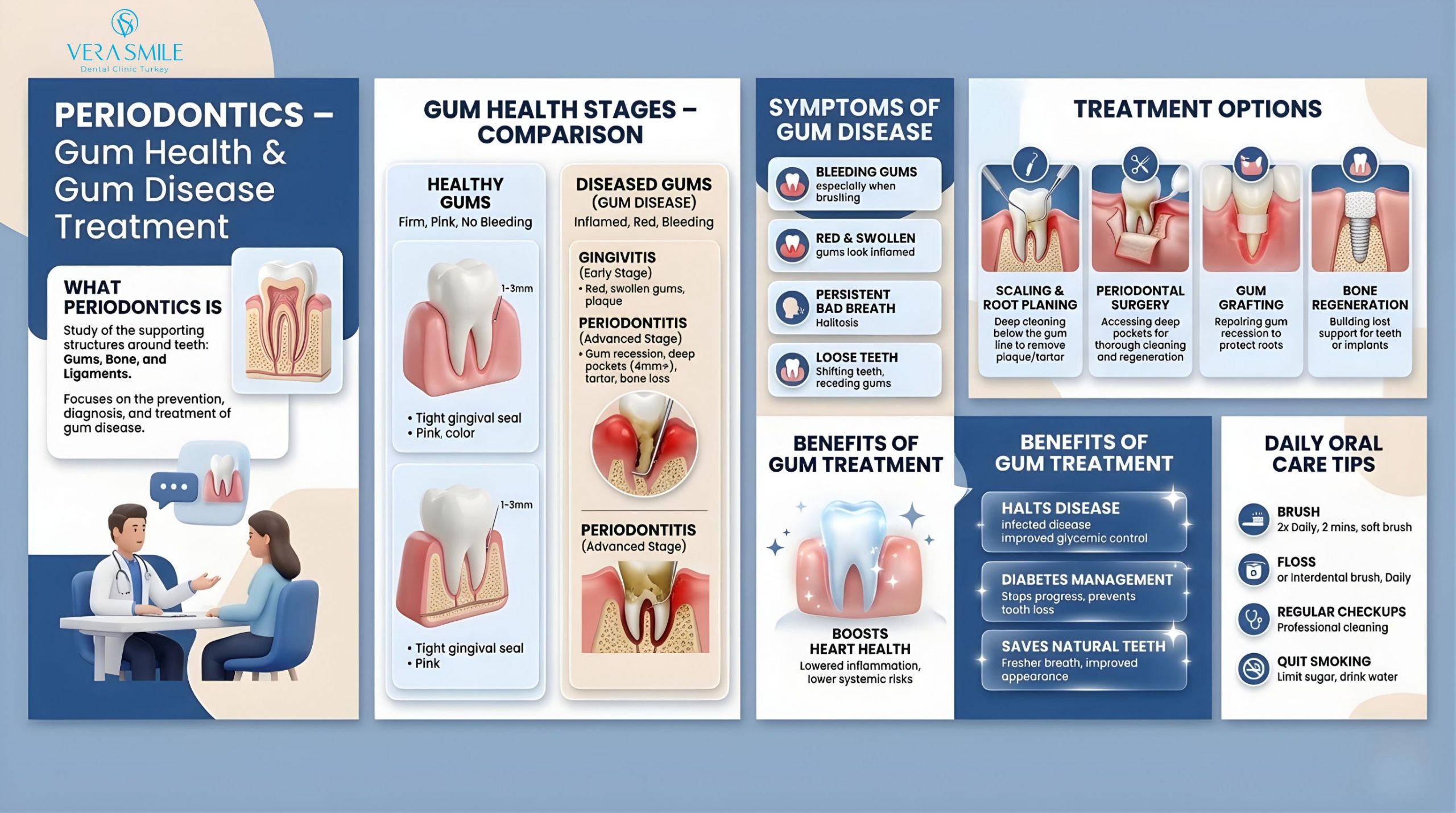
What Are the Periodontal Anatomy and Structures?
The periodontium is a complex system of tissues that not only anchors teeth in place but also protects them from infection and injury. In children, these structures adapt continuously as primary teeth erupt and permanent teeth develop, making their health vital for proper dental growth and function. Below is a detailed overview of the key components of the periodontium and their roles in maintaining strong, healthy teeth.
- Gingiva (Gums): The gingiva is the soft tissue that surrounds the teeth and covers the alveolar bone. It acts as a protective barrier against bacteria and injury, helping to prevent infections such as gingivitis. Healthy gums are firm, pink, and fit snugly around the teeth, providing the first line of defense in oral health. In children, the gingiva also adapts as new teeth erupt, accommodating both primary and permanent teeth.
- Periodontal Ligament (PDL): The periodontal ligament is a network of fibrous connective tissue that attaches the tooth to the alveolar bone. It absorbs and distributes the forces of chewing, acting like a shock absorber for the teeth. The PDL contains nerves and blood vessels that provide sensory feedback and nourishment to the surrounding tissues, which is crucial for proper tooth function and maintenance.
- Cementum: Cementum is a thin, calcified layer that covers the root of the tooth. It serves as the anchor point for the fibers of the periodontal ligament, helping to secure the tooth in its socket. Unlike enamel, cementum can continue to grow slowly over time, allowing minor adjustments to the tooth’s position during growth or after trauma. In pediatric patients, cementum helps guide the proper alignment of erupting permanent teeth.
- Alveolar Bone: The alveolar bone is the part of the jaw that forms the tooth sockets, providing structural support for each tooth. It remodels continuously in response to stress and tooth movement, which is especially important during childhood as the jaw grows and permanent teeth erupt. Healthy alveolar bone is essential for maintaining the stability of both primary and permanent teeth.
- Overall Function: Together, these periodontal structures create a functional unit that stabilizes teeth, protects against infection, supports chewing and speech, and ensures proper oral development. Maintaining the health of the periodontium in children is critical, as early damage or disease can affect tooth alignment, bite development, and long-term oral health.
Why Is Periodontics Important?
Periodontics plays a critical role in preserving not only the health of the mouth but the stability of the entire body. The gums and bone act as the foundation of the teeth, and when these structures are compromised, long-term dental function and aesthetics are put at risk. By focusing on the prevention, diagnosis, and treatment of gum and bone diseases, periodontics safeguards the natural teeth, supports the success of dental implants, and protects against tooth loss, the leading cause of diminished oral function in adults.
Beyond the mouth, the importance of periodontics extends into systemic health. Decades of research have established a close connection between periodontal disease and conditions such as cardiovascular disease, diabetes, respiratory infections, and even imbalances in gut microbiota. Chronic inflammation in the gums allows harmful bacteria to enter the bloodstream, fueling widespread health complications. For patients with existing medical conditions, periodontal care becomes a vital part of overall treatment planning.
From everyday prevention against gingivitis to advanced surgical therapies that regenerate bone and tissue, periodontics ensures that the foundation of the smile remains strong. Its impact goes beyond oral care, it is a cornerstone of long-term wellness, confidence, and quality of life.
How Can Gum Disease Be Prevented?
Gum disease can be prevented through consistent oral hygiene and routine professional care. The most effective prevention strategies include:
- Daily Brushing: Brush twice a day with fluoride toothpaste to remove plaque from tooth surfaces and gumlines.
- Daily Flossing: Clean between the teeth once a day to prevent plaque buildup in hard-to-reach areas.
- Regular Dental Check-Ups: Visit your dentist every six months for exams and professional cleanings to remove tartar.
- Healthy Diet: Limit sugary snacks and acidic drinks that encourage plaque growth and gum irritation.
- Tobacco Avoidance: Avoid smoking or chewing tobacco, as these significantly increase the risk of gum disease.
- Systemic Health Management: Keep conditions like diabetes under control to reduce gum infection susceptibility.
- Antimicrobial Rinses: Use dentist-recommended mouthrinses to lower harmful bacterial levels when needed.
Good daily care combined with routine dental supervision significantly lowers the risk of gingivitis and periodontitis, keeping the gums healthy and stable long-term.
How Is Gum Health Connected to Overall Health?
Gum health is closely linked to overall systemic health. The mouth contains millions of bacteria, and when gum disease develops, these bacteria can enter the bloodstream and contribute to inflammation throughout the body. Strong associations between periodontal disease and conditions such as cardiovascular disease, diabetes, respiratory infections, rheumatoid arthritis, and adverse pregnancy outcomes.
Healthy gums support proper chewing, nutrition, speech, and daily comfort, while gum inflammation can weaken the body’s immune response and worsen existing medical problems. Maintaining good oral hygiene, receiving regular dental cleanings, and treating gum issues early are essential steps for protecting both oral and overall health.
What Are the Common Periodontal Diseases and Conditions?
Periodontal diseases affect the gums and the supporting structures that anchor the teeth in place. They range from mild, reversible inflammation to severe infections that can damage bone and lead to tooth loss. Understanding these conditions helps individuals recognize early warning signs, maintain proper oral hygiene, and seek timely treatment before complications develop.
- Gingivitis: The mildest and most reversible form of gum disease, characterized by red, swollen gums that bleed easily due to plaque accumulation. With early intervention and improved oral hygiene, gingivitis can be fully resolved.
- Chronic Periodontitis: A slow-progressing infection that destroys both gum tissue and the bone supporting the teeth. If left untreated, it can lead to tooth mobility and eventual tooth loss, making early diagnosis essential.
- Aggressive Periodontitis: A rapidly advancing form of gum disease, occurring in younger individuals. It leads to swift bone destruction and requires immediate periodontal care.
- Periodontal Abscess: A painful, localized pocket of pus within the gums caused by bacterial infection. It typically appears suddenly and requires urgent dental treatment to prevent further complications.
- Peri-Implant Mucositis: Inflammation of the soft tissues surrounding a dental implant. Similar to gingivitis, this condition is reversible with proper plaque control and professional cleanings.
- Peri-Implantitis: A more advanced infection around implants involving both soft tissue inflammation and progressive bone loss. Without treatment, peri-implantitis can lead to implant failure.
- Gingival Recession: A condition in which gum tissue recedes or pulls away from the tooth surface, exposing the roots. This increases sensitivity, raises the risk of decay, and affect the appearance of the smile.
What Are the Periodontal Treatments and Procedures?
Periodontal diseases affect the gums and the supporting structures of the teeth, and timely intervention is essential to prevent tooth loss and restore oral health. Depending on the severity of the condition, treatment can range from non-surgical cleanings to advanced surgical and regenerative procedures. The following are the main periodontal treatments commonly used to manage and repair gum disease:
- Scaling and Root Planing: A deep cleaning procedure that removes plaque and tartar from above and below the gumline. Root planing smooths the tooth roots, helping gums reattach and reducing inflammation.
- Gum Surgery (Periodontal Surgery): Used for advanced gum disease when deep pockets cannot be cleaned with non-surgical methods. Techniques include flap surgery to remove bacteria and diseased tissue, or gingivectomy to reshape gums and improve oral health and aesthetics.
- Bone and Tissue Regeneration: Procedures that restore lost bone and gum tissue caused by severe periodontitis. Treatments involve bone grafts, guided tissue regeneration, or growth factors to stimulate natural healing and stabilize teeth.
- Dental Implants and Periodontics: Periodontists manage dental implants, especially when tooth loss results from gum or bone disease. This can include bone augmentation, soft tissue grafts, and ongoing maintenance to ensure long-term implant success.
These procedures aim to halt the progression of gum disease, repair damaged structures, and maintain both the function and appearance of the teeth and gums.
How Periodontics Differ From Other Dental Specialties?
Periodontics stands apart from other branches of dentistry because it focuses specifically on the gums, alveolar bone, and supporting structures of the teeth, rather than the teeth themselves. While general dentists provide preventive care and basic periodontal treatment, a periodontist undergoes additional years of training to diagnose and treat complex gum disease, perform regenerative procedures, and manage dental implants.
This expertise distinguishes periodontics from specialties like orthodontics, which concentrates on tooth alignment and bite correction, or endodontics, which focuses on the inner pulp and root canals of teeth. The difference between a dentist and a periodontist ultimately lies in scope: dentists oversee overall oral care, while periodontists are specialists in preserving the foundation that keeps teeth and implants stable. By addressing the underlying structures of the mouth, periodontics provides the essential groundwork that supports the success of all other dental treatments.
What Is the Difference Between Periodontics vs. Periodontology?
In dentistry, gum health is described using two closely related terms that cause confusion: periodontics and periodontology. Although they are sometimes used as if they mean the same thing, they represent different aspects of the same field. Understanding this distinction provides clarity on how gum science translates into patient care.
Periodontology refers to the scientific study of the periodontium, the gums, periodontal ligament, alveolar bone, and connective tissues that anchor the teeth. It is an academic discipline concerned with research, pathology, and the biological processes that govern both health and disease in these supporting structures. Periodontology lays the foundation for modern understanding of gum disease, bone loss, and regeneration techniques.
Periodontics, by contrast, is the clinical specialty that applies this knowledge in practice. A periodontist translates the science of periodontology into hands-on diagnosis, prevention, and treatment. This includes managing conditions such as gingivitis and periodontitis, performing procedures like scaling and root planing, gum surgery, bone grafting, and placing dental implants when necessary.
In essence, periodontology builds the scientific framework, while periodontics delivers the real-world solutions. One advances knowledge through study, the other restores health through treatment. Together, they form the bridge between research and clinical outcomes, ensuring that patients benefit from the most advanced understanding of periodontal health.
What Is the Difference Between Periodontics vs. Orthodontics
Although both specialties play a vital role in oral health, periodontics and orthodontics address different aspects of care. Periodontics is focused on the health of the gums, alveolar bone, and supporting tissues that hold the teeth in place, emphasizing disease prevention, surgical treatment, and regenerative procedures.
Orthodontics, on the other hand, concentrates on the alignment of teeth and jaws, correcting crowding, spacing, overbites, and crossbites through appliances such as braces or clear aligners.
The two fields often intersect: before orthodontic treatment begins, periodontal health must be stable, since moving teeth in the presence of gum disease accelerate bone loss and worsen recession. Likewise, once orthodontic treatment is complete, healthy gums and bone are essential for maintaining the results. In short, orthodontics aligns the teeth, while periodontics protects and strengthens the foundation that makes alignment stable over a lifetime.
What Is the Difference Between Periodontics vs. Endodontics
While both periodontics and endodontics are dental specialties that treat conditions threatening the survival of teeth, they focus on entirely different areas. Periodontics is dedicated to the tissues surrounding the teeth, the gums, periodontal ligament, and alveolar bone. Its primary concern is managing gum disease, performing regenerative procedures, and ensuring a stable foundation for natural teeth and implants.
Endodontics, in contrast, is concerned with the tissues inside the tooth, specifically the pulp and root canals. Endodontists diagnose and treat pulp infections, most commonly through root canal therapy, to preserve teeth that would otherwise require extraction.
The two specialties often complement one another: a tooth weakened by advanced periodontal disease may also require endodontic treatment, while a tooth saved by root canal therapy still depends on healthy gums and bone to remain functional. Periodontics preserves the external support system, while endodontics protects the inner vitality of the tooth. Together, they play a critical role in extending the lifespan of natural dentition.
What’s the Difference Between a Dentist and a Periodontist?
Both dentists and periodontists play essential roles in maintaining oral health, but their training and areas of expertise differ significantly. A general dentist provides comprehensive care, including preventive services such as cleanings, fillings, crowns, and the early management of gum disease. They act as the first point of contact for most patients, overseeing routine oral care and referring complex cases to specialists when necessary.
A periodontist, on the other hand, is a dentist who has completed additional years of advanced training focused specifically on the gums, bone, and supporting structures of the teeth. This specialization equips them to treat advanced gum disease, perform surgical procedures like gum contouring, bone grafting, and place and maintain dental implants. Periodontists manage complex cases where periodontal disease is linked to systemic conditions such as diabetes or cardiovascular disease.
In simple terms, dentists provide general oral care for overall dental health, while periodontists are the experts who step in when the foundation of the smile, the gums and bone, requires specialized attention.
When Should You See a Periodontist?
Knowing when to seek the care of a periodontist makes the difference between saving natural teeth and facing advanced tooth loss. Since periodontists specialize in the gums, bone, and supporting tissues of the mouth, they are the right professionals to consult when signs of gum disease or structural problems appear. Early intervention not only prevents further damage but also supports long-term oral and systemic health.
- Signs of Gum Disease: Red, swollen, or bleeding gums are among the most common indicators that periodontal health is compromised. If left untreated, these symptoms can progress to gum recession, bone loss, and eventual tooth loss. A periodontist evaluates the extent of disease, measures pocket depth, and provides targeted treatments to halt progression before irreversible damage occurs.
- Persistent Bad Breath or Loose Teeth: Chronic halitosis, or persistent bad breath, often signals bacterial buildup deep below the gumline. In addition, teeth that begin to feel loose, shift position, or change the way they bite together are clear red flags of advanced periodontal disease. Periodontists are trained to diagnose and treat these conditions, restoring both function and confidence.
- Pre-Implant Gum Health Assessment: Before placing a dental implant, it is essential that the gums and bone are strong enough to support the restoration. A periodontist evaluates the health of the supporting tissues, treating gum disease or performing procedures such as a bone graft if necessary. This ensures that the implant has a stable and long-lasting foundation.
- Loose or Shifting Teeth: When teeth begin to feel loose, drift apart, or change the way they bite together, it is a sign that the supporting bone structure has been compromised. This is a hallmark of advanced periodontitis, where bone destruction leads to loss of stability. A periodontist can measure bone loss, perform procedures to regenerate support, and prevent tooth loss. In some cases, splinting or regenerative surgeries may be recommended to stabilize the teeth.
- Deep Periodontal Pockets: During routine dental exams, dentists measure the space between the gum and tooth. Pockets deeper than 3–4 mm are difficult to clean with daily brushing and flossing, creating reservoirs for bacteria and infection. Periodontists specialize in treating these deep pockets through scaling and root planing, pocket reduction surgery, or regenerative therapies to restore healthy attachment and reduce the risk of progression.
- High-Risk Medical Conditions: Systemic conditions such as diabetes, heart disease, or autoimmune disorders increase the severity of gum disease and make healing more difficult. Periodontists are trained to coordinate care with physicians, adapting treatment protocols to manage both oral and systemic health. For example, controlling gum inflammation in a diabetic patient can help improve blood sugar management, creating a two-way health benefit.
- History of Tooth Loss Due to Gum Disease: Patients who have already lost teeth because of gum disease remain at higher risk for losing additional teeth. A periodontist provides ongoing monitoring, specialized maintenance cleanings, and personalized treatment strategies to prevent further progression and stabilize remaining teeth.
