A root canal treatment is a dental procedure that removes infection from the inner part of a tooth, relieves pain, and restores its natural function without extraction. When decay or injury reaches the pulp, bacteria can spread through the root canals, causing inflammation and discomfort. Through precise cleaning, disinfection, and sealing, a root canal eliminates the source of infection and protects the tooth from future damage. Thanks to modern techniques such as microscope-guided endodontics, 3D imaging, and laser disinfection, the procedure is now comfortable, efficient, and highly predictable, allowing patients to keep their natural teeth healthy, strong, and pain-free for years.
What Is a Root Canal Treatment?
A root canal treatment, medically referred to as endodontic therapy, is a dental procedure designed to eliminate infection from within a tooth and protect it from future damage. Inside every tooth lies a chamber called the pulp, a soft tissue composed of nerves, blood vessels, and connective fibers that extend through tiny canals into the root. When decay, trauma, or repeated dental work allows bacteria to penetrate this space, the pulp becomes inflamed or infected. This infection often causes severe pain, lingering sensitivity, or even swelling in the surrounding bone and gums.
Instead of removing the entire tooth, a root canal allows the dentist to preserve the natural structure. The procedure involves carefully removing the infected pulp, cleaning and shaping the canals, and sealing them with a sterile, biocompatible material known as gutta-percha. Once sealed, the tooth is reinforced with a filling or crown, restoring both strength and appearance.
Modern endodontic therapy is guided by microscopic magnification and digital imaging, ensuring every canal is located and disinfected. These technologies have transformed what was once considered a painful treatment into a comfortable, efficient, and highly predictable procedure.
Beyond pain relief, the true purpose of a root canal is to save the natural tooth, maintaining bite balance, preventing bone loss, and preserving the natural aesthetics of the smile. By treating infection at its source, a root canal not only restores oral health but prevents more extensive interventions such as dental implants or dental bridges later on. In essence, it is one of the most conservative and reliable ways to extend the life of a tooth that would otherwise be lost.
Why Is a Root Canal Necessary?
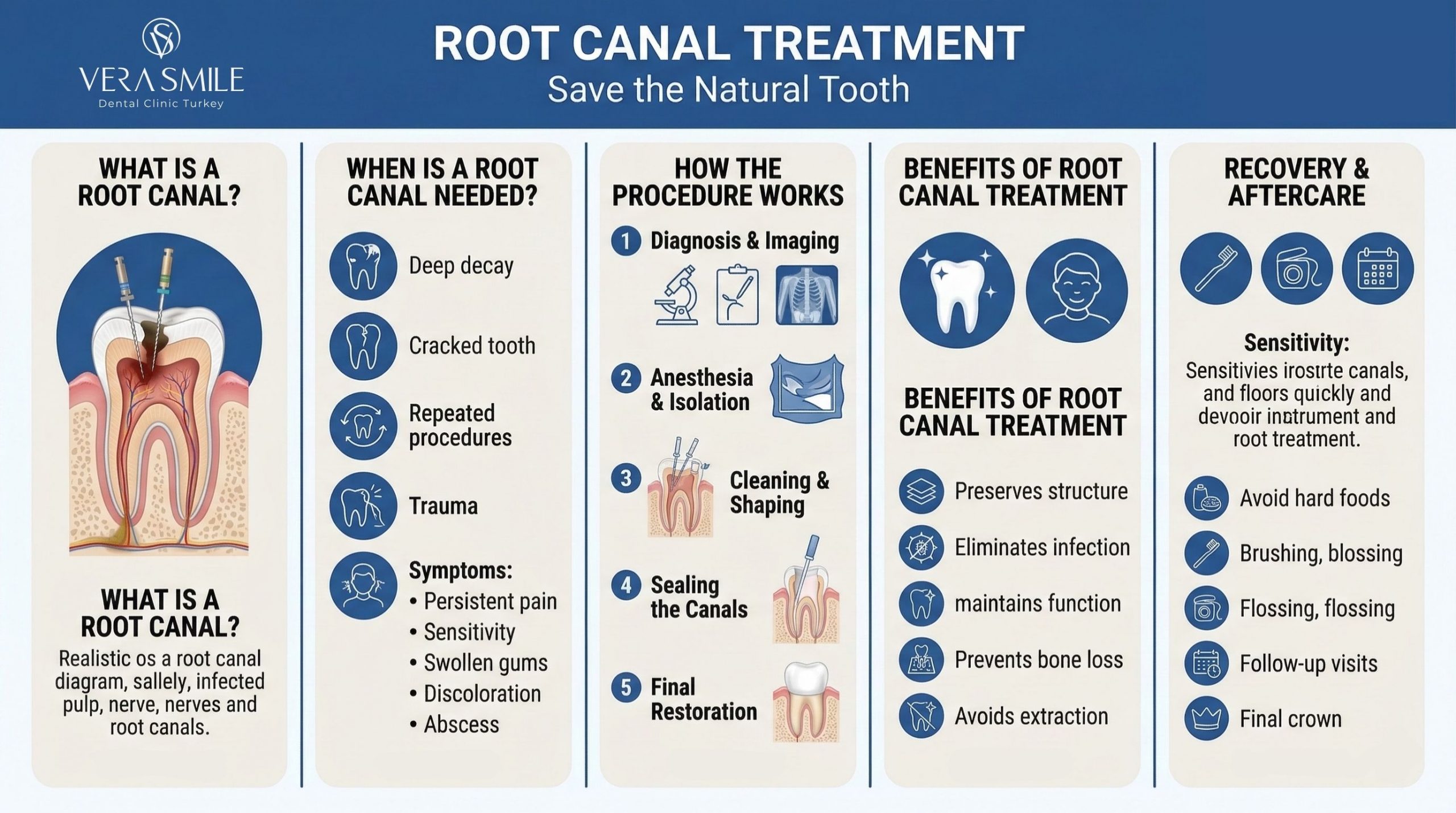
A root canal becomes necessary when the inner tissue of the tooth, the pulp, becomes infected or inflamed. This usually occurs as a result of deep tooth decay, cracks or fractures, traumatic injury, or repeated dental procedures that expose or irritate the pulp. When bacteria enter the pulp chamber, they multiply and cause pressure, inflammation, and infection within the tooth, leading to persistent pain or swelling. Common symptoms that indicate the need for a root canal include:
- Sharp or throbbing tooth pain, especially when biting or chewing
- Prolonged sensitivity to hot or cold even after the source is removed
- Swelling or tenderness in the gums near the affected tooth
- Darkening or discoloration of the tooth
- The appearance of a small pimple-like bump on the gum, indicating an abscess
If left untreated, the infection can spread to surrounding bone and tissue, resulting in gum abscesses, bone loss, and systemic inflammation. In advanced cases, the only alternative may be a tooth extraction. Treating the infection early through endodontic therapy not only relieves pain but preserves the natural tooth, protecting overall oral health and preventing complications related to gum disease and bone deterioration.
How Does a Root Canal Procedure Work Step by Step?
A root canal procedure follows a precise sequence of clinical steps that ensure complete disinfection, sealing, and restoration of the affected tooth. Each stage is designed to remove infection safely and prepare the tooth for long-term strength and aesthetics. The treatment involves several key phases, from diagnostic imaging and anesthesia to cleaning, filling, and final crown placement, all performed under magnification and sterile conditions for maximum accuracy and comfort.
- Diagnosis and Planning: Clinical exams, vitality tests, and digital imaging (periapical X-ray/CBCT) determine the extent of infection and the number/shape of canals. Consent and treatment plan are confirmed.
- Anesthesia and Isolation: Profound local anesthesia ensures comfort. A rubber dam isolates the tooth to keep the field sterile and prevent contamination.
- Access and Pulp Removal: A small access opening exposes the pulp chamber. Under magnification, the dentist locates each canal and removes infected or inflamed pulp tissue.
- Cleaning, Shaping and Disinfection: Rotary nickel-titanium files shape the canals for thorough irrigation. Disinfection uses sodium hypochlorite and EDTA, activated with ultrasonic or laser systems for deep bacterial control. Working length is verified with an electronic apex locator and imaging.
- Filling (Obturation): The canals are dried and sealed hermetically with gutta-percha and a bioceramic sealer using warm vertical condensation or an equivalent technique. A tight seal blocks bacterial re-entry.
- Core Build-Up and Crown Placement:A bonded core restores internal strength. A custom dental crown completes the restoration, protecting the tooth against fracture and restoring function and aesthetics.
Is Root Canal Treatment Painful?
No, modern root canal treatment is not painful. With advanced local anesthesia, patients feel no pain during the procedure, only light pressure. Sedation options can make the experience even more comfortable for those with dental anxiety. Thanks to rotary instruments, digital imaging, and microscope-guided techniques, treatment is quick and gentle.
After the procedure, mild tenderness may appear for 24–48 hours, but it’s easily managed with over-the-counter pain relievers. Overall, today’s root canals are safe, comfortable, and often completed in a single visit.
Root Canal vs Tooth Extraction: Which Is the Better Option?
When a tooth is severely damaged or infected, patients often face a decision between root canal treatment and tooth extraction. While both options remove the source of infection and relieve pain, their long-term effects on function, cost, and aesthetics differ significantly.
A root canal preserves the natural tooth by cleaning and sealing the internal canals, allowing it to continue functioning as part of your natural bite. This approach maintains jawbone integrity, chewing efficiency, and proper alignment of surrounding teeth. It supports natural facial contours, preventing the subtle collapse that can occur when teeth are missing. Once restored with a crown, the treated tooth looks and feels completely natural.
In contrast, a tooth extraction removes the tooth entirely, which initially seems simpler but often leads to secondary complications. Without the tooth root, the jawbone in that area gradually resorbs, causing neighboring teeth to shift and creating gaps that trap food and bacteria. To restore proper function, the missing tooth must be replaced with an implant, bridge, or denture, each of which involves additional time, procedures, and costs.
From a financial perspective, root canal therapy is often the more cost-effective option in the long term. While extraction might appear cheaper initially, the expenses associated with replacement restorations exceed the original treatment. A preserved natural tooth remains the most durable and biologically compatible solution available.
Choosing a root canal over extraction supports better function, aesthetics, and oral health, ensuring the smile remains stable and harmonious for years to come.
Root Canal vs Filling or Crown: Which Treatment Do You Really Need?
Although a root canal, filling, and dental crown all restore damaged teeth, each serves a different purpose depending on how deeply the tooth is affected. Understanding these differences helps determine which treatment best preserves strength, function, and long-term health.
A filling repairs minor to moderate cavities that affect only the outer layers of the tooth, the enamel and dentin, without reaching the inner pulp. The dentist removes decayed material and restores the cavity with composite resin or another restorative material, sealing the surface and restoring normal appearance. Fillings are ideal when decay is shallow and the tooth structure remains strong.
A dental crown is used when a tooth has extensive structural loss or after major restorative procedures. It acts as a protective cap that covers the entire visible portion of the tooth, providing reinforcement and stability. Crowns are often placed after a root canal to prevent fracture and to restore full chewing strength and aesthetics.
A root canal, on the other hand, becomes necessary when infection has reached the pulp, the innermost layer containing nerves and blood vessels. In this case, a simple filling or crown alone cannot remove the infection. The dentist must first clean and seal the canals through endodontic therapy before placing a crown for protection.
In summary, fillings and crowns repair structural or cosmetic damage, while a root canal treats internal infection. When performed in sequence, cleaning the canals and then restoring the tooth with a crown, the result is a fully functional, natural-looking, and long-lasting restoration.
What Should You Do After a Root Canal Treatment?
Proper root canal aftercare is essential for smooth healing and long-term success of the treatment. Once the anesthesia wears off, it’s common to experience mild tenderness or slight sensitivity in the treated tooth or surrounding gums for a day or two. This discomfort is part of the natural healing process and easily managed with over-the-counter pain relief if needed.
During the first 24–48 hours, it’s best to avoid chewing hard or sticky foods on the treated side to prevent pressure on the temporary filling or crown. Soft foods such as soups, yogurt, eggs, or pasta are ideal until the final restoration is placed. Maintaining good oral hygiene is crucial, brush gently around the treated area and continue to floss carefully to keep the gums clean.
Once the final dental crown or permanent restoration is fitted, the tooth will regain full strength and normal chewing function. Scheduling a follow-up visit is important to confirm healing and verify that the bite is correctly adjusted.
To ensure long-term results, patients should:
- Attend routine dental check-ups every 6 months
- Practice daily brushing and flossing
- Avoid biting hard objects such as ice, pens, or nutshells
- Use a night guard if prone to clenching or grinding
With proper care and regular monitoring, a root canal, treated tooth can last a lifetime, maintaining comfort, function, and a healthy, natural appearance.
What Is the Average Cost of a Root Canal in Turkey vs Other Countries?
The cost of a root canal treatment varies significantly depending on the country, the tooth type (front, premolar, or molar), the complexity of the canals, and whether the price includes the final crown restoration. In Turkey and other leading dental tourism destinations, the treatment is performed to European clinical standards at a fraction of the cost found in Western Europe or North America.
| Country | Average Cost (€) | Notes |
| Turkey | 100–250 | Advanced rotary and laser-assisted endodontics; crown extra |
| United Kingdom | 400–700 | Private clinics; endodontist required; crown not included |
| United States | 700–1,200 | Varies by state; insurance coverage limited; crown extra |
| Germany / France | 350–600 | Depends on tooth type and insurance plan |
| India | 60–100 | Economical; quality varies between clinics |
| Mexico | 120–200 | Common for North American dental tourism; crown separate |
How Long Does a Root Canal Take to Heal?
The root canal healing time is generally short, as most patients recover within a few days. After treatment, the surrounding tissue may feel slightly tender or sensitive for 1–2 days, especially while chewing or applying pressure. This is a normal response to the cleaning and disinfection of the inner canals and can be easily managed with mild pain relievers.
By the end of the first week, any residual discomfort typically disappears, and the treated tooth feels completely normal. Once the permanent dental crown or restoration is placed, the tooth regains full strength and function.
A smooth recovery depends on following post-treatment instructions, avoiding hard foods during the initial days, maintaining good oral hygiene, and attending follow-up visits. Persistent pain or swelling beyond a week should be reported to the dentist, as it could indicate residual inflammation or the need for an adjustment.
In most cases, a properly treated and restored tooth heals quickly, remains infection-free, and continues to function comfortably for many years.
What Are the Possible Risks or Complications?
While root canal treatment is one of the most predictable procedures in modern dentistry, certain endodontic complications occur if the infection is not fully eliminated or the restoration is delayed. The most common issues include:
- Reinfection: If bacteria remain inside the canal system or re-enter through a leaking filling or crown, the infection returns. This happen when the tooth has unusually narrow or curved canals that are difficult to access without advanced tools.
- Crown Fracture: A tooth that has undergone root canal therapy becomes more brittle over time because the pulp, which nourished it, is removed. Without a protective dental crown, the tooth can fracture under biting pressure.
- Incomplete Cleaning or Missed Canals: Some teeth, especially molars, have complex internal anatomy with multiple accessory canals. If one remains untreated, infection may persist.
These complications are rare in clinics that use microscope-guided precision, rotary instrumentation, and digital 3D imaging, which allow the dentist to visualize even the smallest canals. Proper sealing with bioceramic materials and timely crown placement further reduce the risk of reinfection.
When performed with modern endodontic techniques such as rotary instrumentation, microscopic guidance, and bioceramic sealing, the success rate of root canal treatment exceeds 90 percent. This finding is supported by clinical research published in the Journal of Endodontics, which confirms that technologically guided root canal therapy achieves high long-term survival rates when paired with proper restoration and follow-up care. Regular dental check-ups and consistent oral hygiene further help the treated tooth remain strong, functional, and infection-free for many years.
