A single dental implant is an artificial tooth root placed into the jawbone to support a custom crown, designed to look and function like a natural tooth. For patients living with a missing tooth, this treatment restores both appearance and oral health, preventing issues such as shifting teeth, bone loss, and difficulty in chewing.
Single dental implants stand out as one of the most reliable tooth replacement options available today. The procedure involves placing a titanium post in the jaw, allowing it to fuse with bone before attaching the final crown. Patients benefit from improved aesthetics, full chewing function, and long-term stability compared to traditional bridges or dentures.
While cost varies depending on the materials of the implant and the crown, region, dentist experience, and the complexity of the case, single implants are widely regarded as a long-term investment in dental health.
What Is A Single Dental Implant?
A single dental implant is used to replace one missing tooth without affecting neighboring teeth. A titanium or zirconia implant is placed into the jawbone, where it integrates with the bone and supports a custom-made crown.
This solution restores natural chewing function, prevents adjacent teeth from shifting, and helps preserve jawbone density. Unlike a dental bridge, a single dental implant stands independently and does not require reshaping healthy teeth.
With proper planning and oral care, success rates exceed 95% over ten years, making it a predictable and long-term tooth replacement option.
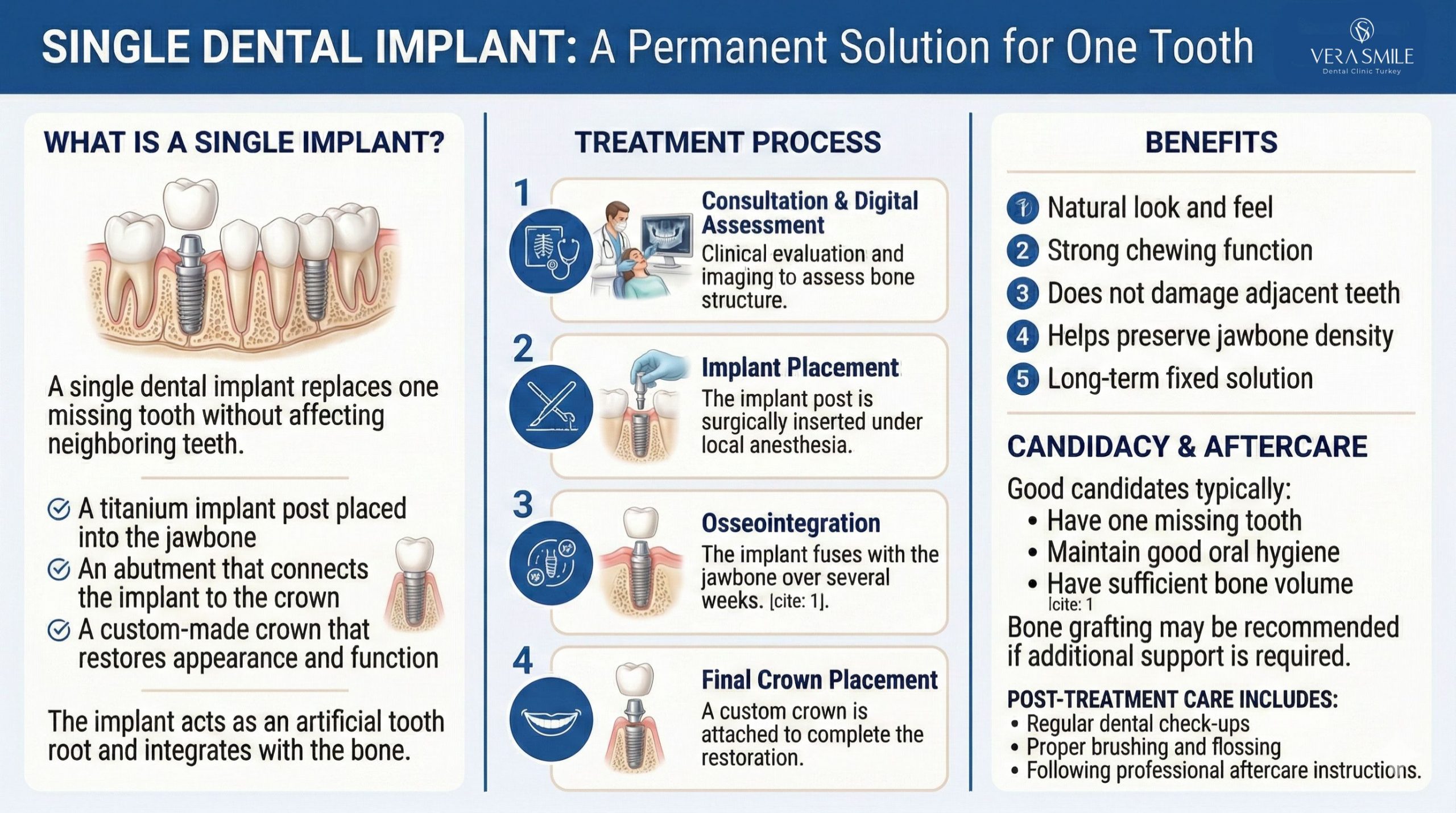
How Does a Single Dental Implant Procedure Work?
A single tooth implant procedure is a structured treatment that replaces a missing tooth with a stable, long-lasting restoration. Instead of sitting on the gums like a denture or relying on neighboring teeth like a bridge, the implant is anchored directly into the jawbone. This gives it the strength and durability of a natural root. The process is divided into several steps:
- Consultation and Imaging: The process begins with a full dental exam, including X-rays or cone beam CT scans. These scans provide a 3D view of the jaw, showing whether the bone has enough height and density for the implant. At this stage, the dentist reviews medical history and discusses treatment options, including bone grafting if the jawbone needs reinforcement.
- Tooth Extraction (if required): If the damaged tooth is still in place, it is removed carefully. In some cases, an implant can be placed immediately after extraction if the bone is healthy enough.
- Implant Placement Surgery: A titanium or zirconia post is surgically inserted into the jawbone. This post acts as the artificial root. A small incision is made in the gum, and a precise hole is drilled into the bone to fit the implant. Once placed, the gum is stitched around the post to allow proper healing.
- Healing and Osseointegration: The most critical phase follows: osseointegration. Over the next 3 to 6 months, the bone cells grow tightly around the implant surface, locking it in place. During this time, a temporary crown or removable prosthesis may be worn for aesthetics and function.
- Abutment Placement: After healing, the gum is reopened to attach an abutment, which connects the implant post to the crown. The gum tissue is then allowed to heal around the abutment for a natural look.
- Crown Attachment: A custom crown designed to match the color, size, and shape of the surrounding teeth is attached. Once in place, the implant feels and functions like a natural tooth.
What Type of Anesthesia Is Used for Single Dental Implants?
Most single dental implant procedures are performed under local anesthesia, which numbs the area while the patient remains awake. The procedure is typically painless, with only mild pressure felt during placement.
For patients with dental anxiety, oral sedation or IV sedation can be added to increase comfort. These methods help patients relax but are used alongside local anesthesia.
General anesthesia is rarely required for a single implant and is usually reserved for complex cases involving multiple implants or advanced surgical procedures.
Before treatment, the dentist reviews the patient’s medical history to determine the safest and most appropriate anesthesia option.
How Long Does a Single Dental Implant Procedure Take?
The timeline for a single implant involves both surgical time and healing time. The surgery itself is efficient, often completed within 30–60 minutes, including preparation, anesthesia, and post-surgical care instructions. If tooth extraction is performed in the same appointment, the procedure may extend to 90 minutes.
The real investment of time comes with healing. Osseointegration, the process where bone fuses to the implant, takes between 3 and 6 months depending on the patient’s age, bone density, and oral health. In cases where the bone is too thin or soft, extra steps such as a bone graft or sinus lift are performed, which can extend the overall treatment timeline to 8–12 months.
What Are the Benefits of Single Dental Implants?
A single dental implant offers more than just a cosmetic fix, it provides a complete, long-term restoration that looks, feels, and functions like a natural tooth. Unlike removable dentures or bridges that depend on adjacent teeth, an implant replaces the entire tooth structure, from root to crown. This approach restores chewing strength, maintains jawbone health, and protects surrounding teeth, making it one of the most reliable and life-enhancing solutions in modern restorative dentistry.
- Natural Appearance: Single dental implants look and feel like real teeth. The custom-made crown is color-matched and shaped to blend seamlessly with the surrounding teeth, restoring a natural smile.
- Restored Chewing Function: Implants provide strong biting force, allowing patients to eat comfortably, from apples to steak, without the slipping or discomfort often caused by dentures.
- Jawbone Preservation: By stimulating the bone like a natural tooth root, implants prevent bone shrinkage and facial collapse, maintaining long-term facial structure and aesthetics.
- Protection of Neighboring Teeth: Unlike bridges, a single implant stands independently, eliminating the need to grind down healthy adjacent teeth for support.
- Long-Term Durability: With proper care, dental implants are among the most predictable treatments in dentistry, showing success rates above 95% after 10 years.
- Improved Speech: The fixed stability of an implant helps maintain clear pronunciation, preventing slurring, lisps, or clicks that removable dentures can cause.
- Boosted Confidence: A secure, lifelike tooth replacement enhances self-esteem, giving patients confidence when speaking, eating, or smiling.
- Easier Oral Hygiene: Implants are cleaned like natural teeth, with regular brushing and flossing, no special tools or adhesives needed.
- Better Bite Alignment: Filling the gap prevents neighboring teeth from drifting, preserving a balanced bite and reducing future dental issues.
- Enhanced Quality of Life: Patients enjoy lasting comfort, freedom from dietary limits, and relief from the frustration of loose dentures or frequent repairs.
What Are the Disadvantages of Single Dental Implants?
While single dental implants are highly successful, the procedure is not entirely free of risks. Most challenges arise during the healing phase or in patients with underlying health conditions. Issues such as bone density, gum health, and adherence to aftercare instructions all play a role in long-term success. In rare cases, complications develop that require additional treatment or adjustments.
- Infection at the Implant Site (Peri-Implantitis): Infection develops when bacteria accumulate around the gums or implant margin, leading to inflammation and bone loss. This condition, known as peri-implantitis, affects approximately 19.5% of patients and 12.5% of implants.
- Nerve Disturbance (Neuropathy): If an implant is placed too close to a nerve, it can cause numbness, tingling, or discomfort in the lips, cheeks, or tongue. Transient neuropathy occurs in about 12% of patients within the first week after surgery, decreasing to 5% after three months. (Prevalence and management of neuropathic injury caused by dental implant insertion in mandible: a systematic review,” Journal of Oral & Facial Pain and Headache 2024)
- Sinus Complications: When implants in the upper jaw extend into the sinus cavity, they may cause sinus pressure, congestion, or infection-like symptoms. Studies report complication rates of 3–5% in maxillary implant cases.
- Implant Failure: Roughly 5% of implants fail within the first year, commonly due to poor osseointegration, smoking, or systemic health issues. When risk factors are well controlled, survival rates exceed 95% after 10 years.
- Mechanical Issues: Technical complications, including loose abutments, screw fractures, or chipped crowns, occur in approximately 7–10% of implants over a 10-year period.
- Bone Loss Around the Implant: Progressive bone resorption compromises implant stability and long-term function. Around 11% of implant sites and 14% of patients exhibit peri-implant bone loss of ≥3 mm.
What Is the Success Rate of Dental Implants?
Dental implants have one of the highest success rates in modern dentistry, thanks to advancements in surgical techniques, implant materials, and digital planning. Clinical research consistently shows implant survival rates of 94–98% over 10 years when placed by qualified specialists and maintained with proper oral hygiene.
Success depends on several factors, including bone quality, patient health, smoking habits, and postoperative care. Implants placed in healthy, non-smoking patients with sufficient bone density can exceed 98% success, while those in medically compromised or heavy-smoking patients may fall to around 85–90%.Dental implants can last for decades when risk factors are managed and proper maintenance is followed, making them one of the most predictable and durable restorative treatments in modern dentistry. This conclusion is supported by Pjetursson et al. (2014) in Clinical Oral Implants Research, which reported long-term survival rates exceeding 95% over ten years.
Who Are Good Candidates for Single Dental Implants?
A single dental implant is ideal for patients with good oral and general health who want to replace one missing tooth permanently. Candidates should have healthy gums, enough jawbone density, and a fully developed jaw to support the implant. Conditions like uncontrolled diabetes, smoking, or active gum disease can increase the risk of complications. Success also depends on a commitment to daily oral hygiene and regular dental check-ups to maintain long-term stability.
- Healthy gums: Stable gum tissue without active periodontal disease is essential for long-term implant success.
- Adequate bone density: A solid foundation in the jawbone allows the implant to integrate securely through osseointegration.
- One missing tooth: The procedure is designed for patients with a single gap that requires restoration, particularly when adjacent teeth remain healthy.
- Good overall health: Conditions like uncontrolled diabetes, heavy smoking, or untreated infections increase the risk of complications, while patients with stable medical profiles generally achieve excellent results.
- Commitment to oral hygiene: Daily brushing, flossing, and regular dental check-ups keep the implant and surrounding tissues healthy for decades.
- Fully developed jaw: Teenagers are advised to wait until jaw growth is complete, since implant placement in an immature jaw compromises stability.
How Much Does a Single Dental Implant Cost?
The cost of a single dental implant varies significantly depending on the country, clinic reputation, and whether additional treatments like bone grafting are required.
| Country/Region | Average Cost (€) |
| Turkey | €450 – €800 |
| India | €500 – €1,000 |
| Mexico | €700 – €1,400 |
| United Kingdom | €2,000 – €3,500 |
| Western Europe (Germany, France, Italy) | €2,200 – €3,800 |
| Australia | €2,000 – €4,000 |
| United States | €3,000 – €4,500 |
Dental implant costs are generally determined by the price of a single implant, influenced by the brand, materials, and crown type. As shown in the table, dental implant cost in Turkey is among the most affordable options worldwide while maintaining the same high quality standards.
What Affects the Dental Implants Single Tooth Cost?
The cost of a single dental implant depends on several factors, including the implant material, treatment complexity, clinic location, and whether additional procedures like bone grafting are needed. Premium brands and advanced technologies may raise the price, while most insurance plans cover only part of the restoration, not the implant itself.
- Implant material: Titanium remains standard, while zirconia costs more.
- Restoration type: A straightforward crown on implant costs less than complex bridges or full-arch work.
- Pre-surgery treatments: A bone graft for dental implant or sinus lift increases overall expense.
- Geographic region: Turkey, India, and Mexico remain lower-cost compared to the US, UK, or Australia.
- Clinic reputation & technology: Premium clinics using Straumann or Nobel Biocare implants charge more.
- Insurance coverage: Most dental plans exclude implants, though some contribute to the crown or abutment costs.
What Is the Aftercare for Single Dental Implants?
To protect healing tissues and ensure long-term success, follow these essential aftercare instructions:
- Pain and Swelling Control: Use cold compresses and take prescribed medication during the first few days to manage discomfort and reduce swelling.
- Dietary Precautions: Avoid hard, sticky, or spicy foods that could irritate or put pressure on the surgical site. Choose soft foods until healing progresses.
- Physical Activity: Limit exercise or heavy movement until your dentist confirms recovery is stable to prevent bleeding or delayed healing.
- Oral Hygiene: Maintain gentle brushing and rinsing, and use implant-specific floss or water irrigators to keep the area clean without disturbing stitches.
- Post-Surgery Care Guidelines: Follow all professional do’s and don’ts to avoid complications such as infection, bleeding, or implant loosening during the healing phase.
What Are the Best Practices for Oral Hygiene After Implant Surgery?
Oral hygiene is the most important factor in preventing infection after implant surgery. Gentle rinsing with saltwater (starting 24 hours after surgery) keeps the surgical site clean. Brushing twice a day with a soft-bristled toothbrush and fluoride toothpaste protects the surrounding teeth and gums. Alcohol-free antibacterial rinses reduce bacteria and gum irritation. Specialized tools such as implant floss threaders, super floss, or water flossers clean under the crown and along the gumline, reducing the risk of peri-implantitis.
How to Manage Pain and Swelling After an Implant
Pain and swelling are the body’s natural response to oral surgery. Applying cold compresses to the cheek near the surgical site during the first 24 hours reduces inflammation by constricting blood vessels. Pain medication, whether prescribed or over-the-counter, should be taken exactly as instructed to keep discomfort under control. Sleeping with the head elevated using two pillows prevents throbbing and speeds recovery. Swelling usually peaks within 48 hours and then decreases. If swelling increases or lasts beyond a week, the dentist should be contacted immediately. at a follow-up appointment.
What Is the Recovery Timeline for Single Dental Implants?
Healing after a single tooth implant takes place in stages. Each phase brings noticeable improvements while moving closer to full restoration.
Cold compress & rest → Manage swelling, mild bleeding, and soreness.
Soft foods only → Yogurt, soups, smoothies.
Medication as prescribed → Pain under control.
Gum healing begins → Tissue closes around the implant.
Stitches removed/dissolve → Dentist follow-up.
Gentle hygiene routine → Brushing, saltwater rinses, implant floss.
Still soft diet → Avoid hard, sticky, or spicy foods.
Osseointegration process → Implant fuses with jawbone.
Temporary crown placed → For aesthetics and light function.
Avoid smoking & alcohol → Protect healing bone.
No excessive bite pressure → Implant still vulnerable.
Full osseointegration complete → Stable implant foundation.
Abutment and crown attached → Final restoration placed.
Normal chewing & speech restored → Feels like a natural tooth.
95%+ success rate at 10 years (source: Clinical Oral Implants Research).
