Tooth loss treatment planning involves structural stability, biological response, and financial commitment, rather than a single preferred solution applied to every case. Dental bridges and dental implants represent two fixed restorative approaches designed to replace missing teeth, restore chewing efficiency, and support facial structure. Despite serving the same restorative purpose, each option relies on a distinct support system that influences surrounding tissues in different ways.
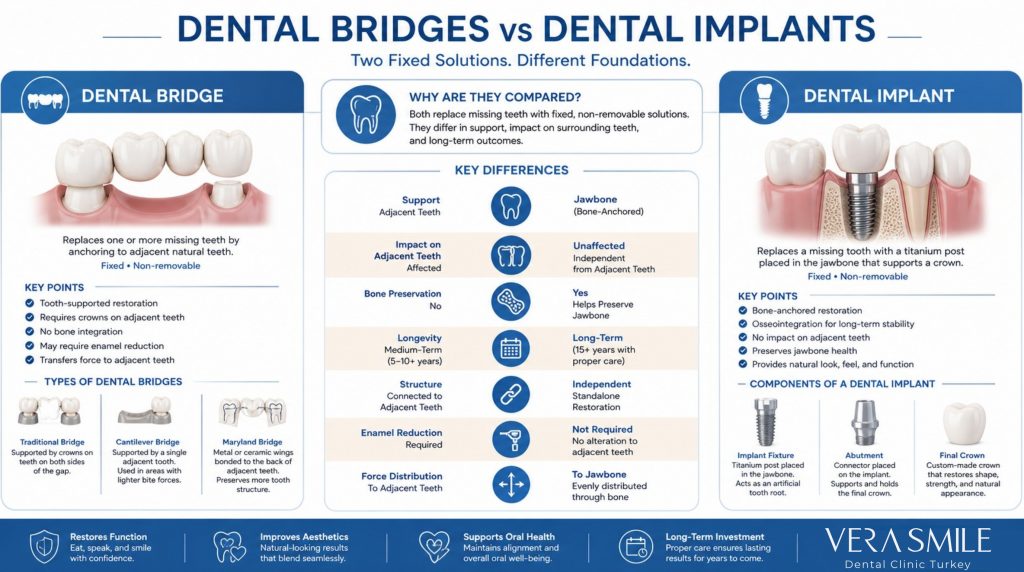
Dental bridges depend on adjacent teeth for retention, creating a connected restoration that spans the missing space. Dental implants rely on direct integration with the jawbone, forming a standalone anchor that functions independently from neighboring teeth. These foundational differences shape how forces are distributed during chewing, how surrounding bone responds over time, and how long the restoration maintains structural integrity.
Understanding how each option interacts with jawbone health, neighboring teeth, treatment duration, and long-term maintenance requirements supports clearer clinical decision-making. This comparison examines dental bridges and dental implants through anatomy, procedure design, cost structure, and long-term outcomes, offering an evidence-based overview without positioning one treatment as superior to the other.
What Defines Fixed Tooth Replacement Options?
Fixed tooth replacement refers to restorations designed to remain permanently attached within the mouth rather than removed for daily cleaning. Dental bridges and dental implants both fall into this category, yet they rely on different anchoring principles. Bridges depend on neighboring teeth for support, while implants transfer functional load directly into the jawbone. These structural differences influence treatment planning, oral hygiene demands, and long-term tissue response. Examining fixed solutions as a category clarifies why bridges and implants serve different clinical roles despite sharing the same restorative goal.
Why Are Dental Bridges and Implants Compared?
Dental bridges and dental implants address tooth loss across both single-tooth gaps and multiple missing teeth. Each treatment delivers a fixed, non-removable restoration, which distinguishes them from removable prosthetic options. This shared functional goal places both approaches within the same clinical decision framework, prompting direct comparison during treatment planning.
The comparison extends beyond surface similarity. Dental bridges rely on tooth-supported retention, while dental implants depend on bone-based anchorage. These different biological foundations influence force distribution, tissue response, and long-term stability. Evaluating bridges and implants side by side clarifies how two fixed solutions achieve restoration through fundamentally different anatomical pathways.
What Decisions Does This Comparison Support?
This comparison helps patients evaluate structural suitability by clarifying how each treatment interacts with existing teeth, bone volume, and bite dynamics. Understanding these structural factors supports realistic expectations regarding stability and restorative design.
The discussion supports financial planning by outlining differences in treatment phases, laboratory involvement, and long-term maintenance demands. Cost evaluation extends beyond initial placement and includes restoration longevity and replacement cycles.
Assessing the long-term oral health impact highlights how each option influences bone preservation, adjacent teeth, and functional balance over time. Viewing these outcomes together allows patients to approach treatment selection through clinical context rather than preference-driven assumptions.
What Is a Dental Bridge?
A dental bridge is a fixed restorative structure designed to replace one or more missing teeth by spanning the gap between existing natural teeth. The restoration gains support from adjacent teeth, which receive dental crowns that anchor the artificial tooth or teeth positioned between them. This design creates a single connected unit that restores chewing function and maintains tooth alignment.
Dental bridges function without direct anchorage in the jawbone. Stability depends on the strength and condition of the supporting teeth, as well as precise crown preparation. By restoring the space left by tooth loss, a dental bridge supports speech clarity, bite balance, and visual symmetry while relying on tooth-based retention rather than bone integration.
How Does a Dental Bridge Replace Missing Teeth?
A dental bridge replaces missing teeth by forming a fixed structure that spans the empty space within the dental arch. The artificial tooth occupies the gap created by tooth loss, restoring continuity along the bite line. Stability comes from neighboring teeth that anchor the restoration, allowing the bridge to function as a single connected unit during chewing and speaking.
This approach restores contact between opposing teeth, limits unwanted tooth movement, and supports facial symmetry. Because the restoration remains fixed in place, daily function resembles that of natural teeth while relying entirely on tooth-based support rather than jawbone integration.
What Role Do Adjacent Teeth Play in a Dental Bridge?
Adjacent teeth serve as the primary support system for a dental bridge. These teeth undergo preparation to receive crowns that hold the restoration in position. Their strength, alignment, and periodontal condition influence how chewing forces transfer across the bridge.
During function, pressure passes from the artificial tooth to the crowned supporting teeth. This load-sharing role places structural demand on the adjacent teeth, making their long-term health central to bridge performance.
How Does a Crown-Based Support Structure Work?
A crown-based support structure involves reshaping the anchoring teeth to allow precise crown placement. These crowns form the attachment points that secure the bridge and maintain positional stability. Accurate crown margins support comfort, bite balance, and predictable wear patterns.
Once cemented, the crowns lock the restoration into place and prevent independent movement of the replacement tooth. The entire unit functions together, with force distribution guided by the supporting teeth.
What Types of Dental Bridges Are Used in Clinical Practice?
Dental bridges follow distinct structural designs based on how support is achieved and how chewing forces transfer through the restoration. Each design serves a specific clinical role defined by tooth position, load direction, and available anchorage.
- Traditional Fixed Bridge: This design uses two natural teeth positioned on either side of the missing tooth. Full-coverage crowns placed on these teeth secure the artificial tooth between them. Force distribution spreads across both anchors, supporting balanced function and positional stability.
- Cantilever Bridge: This bridge relies on a single adjacent tooth for support. The artificial tooth extends outward from one anchored crown, concentrating functional load on one structure. Placement aligns with areas exposed to reduced bite pressure due to the focused load pattern.
- Maryland (Resin-Bonded) Bridge: This design attaches to neighboring teeth through thin metal or ceramic wings bonded to inner tooth surfaces. Full crown preparation is avoided, preserving natural tooth structure. Retention depends on adhesive bonding and precise enamel contact.
What Is a Dental Implant?
A dental implant is a fixed tooth replacement that restores a missing tooth through direct anchorage within the jawbone. The system consists of a titanium post placed into bone tissue, serving as an artificial root that supports a prosthetic crown. This structure allows the restoration to function independently from neighboring teeth.
Dental implants rely on a biological bonding process between bone and implant surface, creating a stable foundation for chewing forces. By transferring load into the jawbone, the implant supports bite stability and preserves spatial balance within the dental arch. The restoration remains fixed in place and functions as a standalone unit rather than a connected structure.
How Do Dental Implants Function Within the Jaw?
Dental implants function as artificial tooth roots anchored inside the jawbone. Their stability depends on biological integration rather than mechanical attachment, creating a load-bearing structure that responds to chewing forces in a controlled and predictable manner.
What Is the Role of the Titanium Implant Post?
The titanium implant post serves as the core anchoring element placed within the jawbone. Titanium’s biocompatibility allows direct contact with bone tissue without triggering immune rejection. The post transfers chewing forces into the jaw, mimicking the functional behavior of a natural tooth root while preventing localized bone collapse.
How Does the Osseointegration Process Work?
Osseointegration refers to the biological fusion between bone cells and the implant surface. During this phase, bone tissue grows directly onto the micro-textured titanium surface, creating structural continuity. This bond stabilizes the implant, eliminates micromovement, and enables long-term functional loading without connective tissue interference.
What Are the Core Components of a Dental Implant System?
A dental implant system is built from distinct structural elements, each designed to perform a specific clinical role within the restoration process.
- Implant Fixture: The implant fixture is the root-form component placed directly into the jawbone. It provides primary stability and transfers chewing forces into bone tissue, supporting long-term load distribution and structural balance within the dental arch.
- Abutment: The abutment connects the internal implant fixture to the visible restoration. It defines the emergence profile, supports soft tissue contouring, and creates a secure interface between the implant body and the crown.
- Final Crown: The final crown restores tooth shape, surface texture, and bite function. Fabricated from ceramic or zirconia materials, it delivers wear resistance, color integration, and functional contact with opposing teeth while completing the implant system’s restorative phase.
How Do the Structural Designs of Dental Bridges and Implants Differ?
Dental bridges and dental implants differ at a fundamental structural level based on how each restoration gains support within the mouth. A dental bridge relies on adjacent natural teeth as anchoring units, using crowns or bonded frameworks to span the missing tooth space. The load created during chewing transfers through these supporting teeth rather than into the jawbone beneath the missing area.
Dental implants use a bone-anchored foundation that replaces the tooth root itself. The implant fixture integrates within the jaw, allowing chewing forces to disperse through bone tissue instead of neighboring teeth. This structural independence preserves the position and integrity of surrounding teeth while maintaining internal load balance across the dental arch.
These design differences influence stress distribution, long-term stability, and how each option interacts with bone volume and soft tissue architecture.
How Do Dental Bridges and Implants Differ in Their Support Mechanisms?
Dental bridges and dental implants rely on distinct support strategies that determine how biting forces travel through the oral structures. A dental bridge gains stability from neighboring teeth, which are prepared to carry the load of the missing tooth area. These teeth function as anchors, absorbing functional pressure through crowned or bonded connections.
Dental implants obtain support through direct integration with the jawbone. The implant fixture serves as an artificial root, transferring functional forces into bone tissue rather than into adjacent teeth. This support model creates a self-sustaining structure that remains independent within the dental arch and maintains mechanical balance during daily function.
How Do Tooth-Supported Restorations Function?
Tooth-supported restorations rely on natural adjacent teeth to stabilize the replacement tooth. These teeth receive crowns or bonding frameworks that secure the bridge in place. Functional pressure transfers through the supporting teeth during chewing, placing them under continuous mechanical demand.
How Do Bone-Anchored Restorations Function?
Bone-anchored restorations gain stability through direct fixation within the jawbone. The implant fixture acts as a substitute tooth root, allowing chewing forces to disperse through bone structure. This anchorage creates an independent support system that does not rely on neighboring teeth for stability.
How Do Dental Bridges and Implants Impact Adjacent Teeth?
Dental bridges influence adjacent teeth through direct structural dependence. The neighboring teeth require reshaping to support crowns or retainers, placing them under continuous functional load during chewing and biting. This dependency alters how these teeth absorb pressure and maintain long-term structural integrity.
Dental implants remain independent from surrounding teeth. The restoration gains stability from the jawbone rather than from adjacent enamel surfaces. This separation preserves natural tooth structure and prevents added mechanical stress on neighboring teeth during daily function.
What Enamel Reduction Is Required for Dental Bridges and Implants?
Dental bridges require controlled enamel reduction on neighboring teeth to allow crown placement and structural retention. This preparation permanently alters the supporting teeth and assigns them a load-bearing role within the restoration.
Dental implants require no enamel modification of adjacent teeth. The implant fixture secures directly within the jawbone, preserving surrounding tooth structure while maintaining independent support.
How Does Load Distribution Differ Between Dental Bridges and Implants?
Dental bridges direct chewing forces through the adjacent support teeth, concentrating mechanical stress within the crowned units that anchor the restoration. These teeth absorb pressure created by the missing tooth space during daily function.
Dental implants transfer functional forces into the jawbone itself, allowing stress to disperse through bone structure rather than neighboring teeth. This distribution supports mechanical balance across the dental arch and preserves adjacent tooth integrity.
How Do Dental Bridge and Implant Treatment Processes Differ?
The treatment process for dental bridges and dental implants follows distinct clinical pathways based on structural design and biological involvement. A dental bridge procedure centers on adjacent tooth preparation, impression taking, and prosthetic fabrication. Once the supporting teeth receive shaping, crowns or retainers secure the bridge framework, allowing restoration within a relatively short treatment window.
Dental implant treatment follows a surgically driven sequence. The process begins with implant placement into the jawbone, followed by a healing phase where bone integration establishes internal stability. After integration, a connecting component and final crown complete the restoration. This staged approach prioritizes biological adaptation and long-term anchorage rather than immediate prosthetic attachment.
These differences influence treatment duration, clinical steps, and the level of biological involvement required for each option.
What Clinical Steps Are Involved in Dental Bridge Treatment?
Dental bridge treatment follows a structured prosthetic sequence designed around the supporting teeth.
- Anchor Tooth Assessment: Adjacent teeth undergo clinical and radiographic evaluation to confirm structural strength and suitability for load-bearing support.
- Tooth Preparation: Selected support teeth receive controlled reshaping to create space for crowns or retainers that will secure the bridge framework.
- Impression and Bite Recording: Accurate impressions capture tooth alignment and occlusal relationships, guiding precise laboratory fabrication.
- Temporary Bridge Placement: A provisional bridge preserves spacing, function, and appearance while the definitive restoration is produced.
- Final Bridge Delivery: The finished bridge is fitted, occlusion is refined, and the restoration is permanently secured to complete treatment.
What Clinical Steps Define the Dental Implant Treatment Process?
Dental implant treatment follows a biologically driven sequence focused on surgical placement and tissue integration.
- Diagnostic Planning: Clinical examination and imaging define bone volume, anatomical landmarks, and implant positioning to support long-term stability.
- Implant Placement: The implant fixture is surgically inserted into the jawbone at a planned depth and angle to establish primary stability.
- Healing and Bone Integration: A dedicated healing phase allows bone tissue to integrate with the implant surface, creating internal anchorage within the jaw.
- Abutment Connection: After integration, an abutment is secured to the implant fixture to support soft tissue shaping and prosthetic attachment.
- Final Crown Placement: The definitive crown is fabricated and attached, restoring bite function, tooth form, and aesthetic continuity.
How Do Dental Bridge and Dental Implant Costs Compare?
Before reviewing numerical differences, cost evaluation between dental bridges and dental implants requires an understanding of what each price reflects clinically. Treatment fees represent more than materials alone; they account for procedural complexity, number of treated teeth, laboratory involvement, and long-term service life. A bridge concentrates cost across multiple prepared teeth, while an implant separates surgical and restorative components into distinct financial stages. This comparison outlines how pricing forms for each option and how long-term cost impact relates to durability and maintenance rather than initial payment alone.
| Cost Category | Dental Bridge | Dental Implant |
| Initial Procedure Cost | Lower upfront cost due to prosthetic-focused treatment | Higher upfront cost due to surgical placement and implant components |
| Number of Teeth Involved | Costs increase with each supporting tooth and pontic unit | Cost calculated per missing tooth or implant-supported restoration |
| Laboratory Fees | Multiple crowns and bridge framework fabrication | Single crown fabrication with implant-specific components |
| Surgical Costs | No surgical placement required | Surgical fee included for implant insertion |
| Maintenance Expenses | Higher long-term repair or replacement costs | Lower long-term intervention due to independent support |
| Replacement Cycle | Shorter lifespan requiring future replacement | Extended functional lifespan with proper care |
| Overall Long-Term Cost Impact | Recurrent costs linked to supporting teeth | Cost efficiency improves over extended time span |
What Are the Longevity and Maintenance Requirements of Bridges and Dental Implants?
The longevity and maintenance requirements of bridges and dental implants differ due to how each restoration is supported and how it interacts with surrounding tissues.
| Criteria | Dental Bridge | Dental Implant |
| Average Lifespan | Approximately 7–15 years | Frequently 20+ years with stable bone support |
| Structural Support | Anchored to adjacent teeth | Anchored directly into the jawbone |
| Load Distribution | Supporting teeth absorb chewing forces | Implant transfers force into the bone |
| Primary Risk Factor | Decay or periodontal disease affecting abutment teeth | Peri-implant tissue inflammation or bone loss |
| Hygiene Requirement | Cleaning under the pontic and around supporting teeth | Cleaning around the implant crown and gum margin |
| Professional Monitoring | Evaluation of margins, supporting teeth, and structural integrity | Assessment of bone levels and soft tissue health |
| Component Replacement | Entire bridge replaced if structural failure occurs | Crown may require replacement; implant fixture remains in place |
When Does a Dental Bridge Meet Clinical Criteria?
Determining whether a dental bridge represents an appropriate treatment option requires careful evaluation of surrounding teeth and local anatomical conditions. Since a bridge depends on adjacent teeth for structural support rather than bone integration at the missing tooth site, both tooth integrity and tissue stability influence clinical suitability.
- Condition of Neighboring Teeth: A dental bridge requires adjacent teeth with strong structural integrity and sufficient enamel and dentin thickness to support crown preparation. Teeth affected by extensive decay, fractures, or large restorations present reduced reliability as abutments. Stable periodontal support remains essential, since gum attachment and surrounding bone determine long-term retention. When neighboring teeth already require crowns, incorporating them into a bridge design aligns with restorative treatment planning.
- Local Bone Structure Considerations: Bridge placement does not depend on bone integration at the missing tooth site, yet ridge contour and soft tissue volume influence aesthetic and functional outcomes. Adequate gum support allows proper pontic design and natural emergence profile. Severe ridge collapse affects visual harmony and hygiene access, requiring soft tissue management or ridge modification to improve structural balance.
When Do Dental Implants Meet Clinical Criteria?
Selecting dental implants as a treatment option requires evaluation of bone structure and overall biological health. Since an implant functions as an artificial tooth root anchored directly within the jaw, both bone quality and systemic healing capacity determine clinical suitability.
- Jawbone Density and Volume: Dental implants require sufficient bone height, width, and density to achieve primary stability at placement. Strong bone structure supports successful osseointegration and long-term load distribution. Inadequate bone volume compromises anchorage and mechanical stability. In such cases, bone grafting procedures restore structural foundation before implant insertion.
- Systemic Health and Healing Factors: Implant success depends on stable healing response and controlled systemic conditions. Well-managed diabetes, absence of active periodontal infection, and strong oral hygiene practices support predictable integration. Uncontrolled systemic disease, heavy smoking, or immune suppression interferes with bone healing and increases complication risk. Comprehensive medical and dental assessment determines whether implant therapy aligns with the patient’s biological profile.
How Do Dentists Choose Between a Bridge and an Implant?
Replacing a missing tooth requires more than a cosmetic decision. Dentists evaluate oral health, structural support, and long-term stability before recommending a bridge or an implant. Each option restores function and appearance, yet the right choice depends on clinical findings and patient priorities.
- Bone Density: Adequate jawbone volume supports implant placement, since the post must fuse with the bone. Limited bone height or width points toward a bridge when grafting is not part of the plan.
- Gum Health: Healthy gums create a stable environment for long-term implant success. Active periodontal disease shifts the recommendation toward stabilizing oral health first or selecting a bridge.
- Condition of Adjacent Teeth: A bridge depends on nearby teeth for support. Teeth with large restorations fit well under bridge crowns. Intact, healthy teeth favor implant placement to avoid reshaping natural enamel.
- Number of Missing Teeth: A single missing tooth suits an implant when bone support remains strong. Multiple missing teeth in a row align well with a bridge design anchored to prepared teeth.
- Medical History: Surgical placement requires stable overall health. Conditions that affect healing, such as uncontrolled diabetes or immune disorders, influence the decision toward a non-surgical option.
- Treatment Timeline: Implant therapy involves placement, healing, and crown attachment across several months. A bridge delivers restoration in fewer visits.
- Longevity Goals: Implants function as artificial roots and maintain jawbone stimulation. Bridges restore chewing ability and appearance while relying on supporting teeth for durability.
- Budget Considerations: Implant treatment carries higher upfront cost due to surgical steps and materials. Bridges require lower initial investment and shorter chair time.
Is a Dental Implant More Invasive Than a Bridge?
Yes. A dental implant involves a surgical procedure. The dentist places a titanium post into the jawbone to replace the missing tooth root. This step requires local anesthesia, precise planning, and a healing period while the bone integrates with the implant. Mild swelling and discomfort follow the placement phase.
A dental bridge does not require surgery. The dentist reshapes the adjacent teeth and places crowns to support the artificial tooth between them. This process focuses on tooth preparation rather than bone placement. Recovery remains limited to minor sensitivity around the prepared teeth.
Invasiveness relates to the area being treated. An implant affects bone and soft tissue at the missing tooth site. A bridge impacts the structure of neighboring teeth. Each option changes different parts of the mouth, and dentists base their recommendation on clinical evaluation and long-term goals.
Which Option Influences Bone Loss?
A dental bridge influences bone loss more than a dental implant. An implant integrates with the jawbone and transfers chewing forces into the surrounding tissue, which helps maintain bone structure. A bridge does not replace the tooth root. The area beneath the artificial tooth receives no direct stimulation, which leads to gradual bone reduction over time.
Does Age Affect Treatment Selection?
Yes. Age affects treatment selection, though oral health and bone condition guide the final decision. Younger patients must complete jaw development before implant placement. Active bone growth influences implant stability, so dentists wait until skeletal maturity.
Older adults qualify for implants or bridges based on bone density, gum health, and medical history. Strong bone support and stable systemic health support implant placement in later years. When bone volume declines or healing capacity decreases, a bridge provides a reliable alternative. Dentists focus on biological health rather than chronological age alone.
Which Treatment Requires More Time to Complete?
A dental implant requires more time to complete than a dental bridge.Implant treatment includes surgical placement of the titanium post, followed by a healing phase that allows the bone to integrate with the implant. After integration, the dentist attaches the final crown. This process spans several months. A dental bridge involves reshaping adjacent teeth and placing crowns to support the artificial tooth. The restoration is completed within a few appointments, with no surgical healing period required.