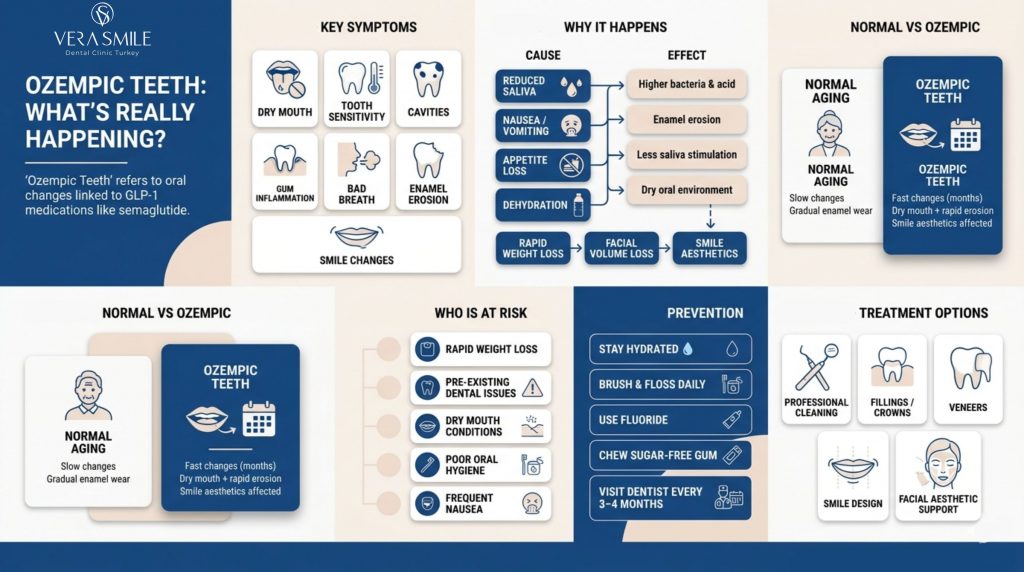
Ozempic Teeth refers to a range of oral health and aesthetic changes, including dry mouth, enamel erosion, gum sensitivity, and altered smile appearance, observed in people using GLP-1 receptor agonists such as semaglutide (Ozempic, Wegovy). While the term is not yet a formal clinical diagnosis, it has gained significant traction among patients, dentists, and researchers as reports of dental side effects linked to GLP-1 medications continue to rise. The conversation matters because millions of people worldwide are now using these medications, and their oral health implications are only beginning to be understood.
Is Ozempic Teeth a Real Medical Condition or a Social Media Myth?
Ozempic Teeth is not an officially classified medical condition, but it is not simply a social media myth either. It describes a real pattern of oral health changes that dentists are beginning to notice in patients on GLP-1 medications. The term emerged organically from patient reports and clinical observations, not from a single published study. However, emerging research and case reports support the biological plausibility of these changes.
A 2024 pharmacovigilance analysis published in academic literature identified dry mouth (xerostomia), salivary gland dysfunction, and oral infections as adverse events reported in association with semaglutide use. These findings suggest that while Ozempic Teeth may be a social media-coined phrase, the underlying dental concerns it describes have a legitimate clinical basis.
Is Ozempic Teeth Different from Normal Dental Aging?
Yes, and the distinction matters. Normal dental aging involves gradual enamel thinning, gum recession, and tooth discolouration over decades. Ozempic Teeth, by contrast, can develop over months, particularly in patients experiencing rapid weight loss, dehydration, or changes in eating habits. The accelerated timeline and the specific combination of symptoms, especially dry mouth alongside sudden facial volume loss, set it apart from routine age-related dental changes.
How Does Ozempic Affect Oral Health?
Ozempic affects oral health through several direct and indirect mechanisms. GLP-1 receptors are present in salivary glands, meaning semaglutide can directly influence saliva secretion. Reduced saliva production lowers the mouth’s natural defences against acid, bacteria, and plaque, creating conditions that accelerate tooth decay, enamel erosion, and gum disease.
Ozempic commonly cause nausea and vomiting, particularly during dose escalation. Frequent vomiting exposes tooth enamel to stomach acid, a well-established driver of enamel erosion. The drug’s appetite-suppressing effects also change eating patterns, often reducing nutrient intake in ways that indirectly affect gum and bone health.
How Could Ozempic Indirectly Affect Oral Health?
Beyond its direct action, Ozempic influences several systemic factors that can indirectly affect oral health. These include changes such as reduced appetite, dehydration, and rapid weight loss, all of which have downstream consequences for saliva production, enamel protection, and gum health. The key indirect factors include:
- Reduced Appetite: Less chewing and smaller meal volumes reduce mechanical stimulation of saliva.
- Dehydration: Lower fluid intake or nausea-related fluid loss decreases salivary output.
- Rapid Weight Loss: Changes in facial fat and soft tissue support can alter the appearance of teeth and smile aesthetics.
These mechanisms collectively increase vulnerability to enamel erosion, gum inflammation, and aesthetic changes in the smile. Understanding them helps patients and dentists take preventive measures before significant damage occurs.
Does Reduced Appetite Impact Saliva Production?
Yes. Saliva production is partly stimulated by chewing and eating. When Ozempic significantly reduces appetite, and therefore meal frequency and food volume, the mechanical stimulation needed to maintain healthy salivary flow decreases. Less saliva means a drier oral environment, higher acid concentration, and reduced antimicrobial protection, all of which increase the risk of tooth decay and oral infections.
Can Dehydration from Ozempic Affect Teeth?
Dehydration is a frequently reported side effect of Ozempic, often linked to nausea-related fluid loss or simply to reduced thirst perception. Chronic low-grade dehydration compounds dry mouth significantly. Saliva is 99% water, and even mild systemic dehydration can reduce salivary volume and change its composition, making it less effective at buffering acids and remineralising enamel.
Is There a Link Between Weight Loss and Facial Volume Loss?
Yes, and this is where the cosmetic dimension of Ozempic Teeth becomes relevant. Rapid, significant weight loss, especially when it occurs quickly, leads to loss of subdermal facial fat. This affects cheek volume, lip support, and the structural padding around the jaw. As these soft tissue volumes diminish, the teeth can appear more prominent, the smile can look uneven, and overall facial harmony can be disrupted. This phenomenon overlaps closely with what is widely known as “Ozempic Face.”
Who Is More Likely to Experience Ozempic Teeth?
Not every person taking Ozempic will develop notable dental issues, but certain profiles carry higher risk. Patients who experience significant weight loss rapidly, those who were already managing dental conditions prior to starting the medication, and individuals who develop persistent nausea or dry mouth are at the greatest risk of compounding oral health problems. Other risk factors include:
- Pre-existing dry mouth conditions (Sjögren’s syndrome, medication-induced xerostomia)
- High baseline sugar intake combined with reduced saliva
- Irregular dental care habits before starting GLP-1 therapy
- Older age, where enamel and gum tissue are already more vulnerable
- Rapid, substantial weight loss (over 10–15% of body weight in a short period)
Patients in these categories should be especially vigilant about oral health and consult their dentist proactively.
Are Existing Dental Issues a Risk Multiplier for Ozempic Teeth?
Definitively yes. A patient with pre-existing gum disease, exposed root surfaces, or weakened enamel enters a more vulnerable baseline state. When Ozempic then reduces saliva flow and introduces acid exposure from nausea or vomiting, these existing vulnerabilities are amplified. Dentists consistently observe that patients with prior dental disease experience faster progression of oral problems when systemic factors like dehydration and dry mouth are introduced.
Why Are Dental Side Effects Being Linked to Ozempic?
Several converging biological and behavioural mechanisms explain the dental side effects associated with Ozempic use:
- GLP-1 receptor activity in salivary glands: Semaglutide activates GLP-1 receptors found in salivary tissue, potentially disrupting normal saliva secretion.
- Nausea and acid exposure: Up to 20% of Ozempic users experience nausea or vomiting, particularly early in treatment, repeatedly exposing enamel to stomach acid.
- Reduced eating frequency: Less chewing means less mechanical saliva stimulation, lowering overall salivary output.
- Systemic dehydration: Fluid loss from gastrointestinal side effects reduces whole-body hydration, including salivary gland output.
- Nutritional changes: Reduced appetite can lead to lower intake of calcium, vitamin D, and other nutrients essential for tooth and bone health.
- Rapid weight loss: Fast fat loss changes facial structure and soft tissue support, altering smile appearance aesthetically.
Understanding these mechanisms allows dentists to create targeted preventive and restorative strategies for patients on Ozempic.
What Are the Signs of Ozempic Teeth?
The signs of Ozempic-related dental changes tend to cluster around dryness, sensitivity, and aesthetic shifts. Patients and clinicians should watch for the following:
- Persistent dry mouth: A consistently parched feeling, even without obvious dehydration
- Increased tooth sensitivity: Especially to cold, hot, or sweet foods, an early indicator of enamel thinning
- Frequent cavities: A sudden rise in decay in patients without a prior history of dental problems
- Gum inflammation or bleeding: Redness, puffiness, or bleeding when brushing
- Bad breath (halitosis): Dry mouth reduces the cleansing action of saliva, allowing odour-causing bacteria to proliferate
- Visible enamel wear or translucency: Teeth appear thinner or more see-through at the edges
- Teeth appearing smaller or more worn: An aesthetic change linked to enamel loss or shifting facial proportions
- Oral infections or thrush: Reduced salivary immunity can allow fungal or bacterial overgrowth
Early recognition of these signs is critical for preventing more severe dental complications.
Does Ozempic Cause Dry Mouth?
Yes, dry mouth (xerostomia) is one of the most consistently reported oral side effects among Ozempic users. It results from the combined effect of GLP-1 receptor activity in salivary glands, reduced fluid intake, and systemic dehydration from gastrointestinal side effects. Persistent dry mouth is not merely uncomfortable, it fundamentally disrupts the mouth’s self-cleaning and buffering capacity.
Can Ozempic Lead to Bad Breath?
Ozempic can contribute to bad breath through two pathways. First, reduced saliva allows oral bacteria to thrive and produce sulphur compounds that cause halitosis. Second, patients in a caloric deficit may enter mild ketosis, which produces a distinct acetone-like breath odour. Together, these factors can make bad breath a noticeable and socially distressing side effect for some users.
Does Ozempic Affect Gum Health?
Ozempic can negatively affect gum health, primarily through the mechanism of dry mouth. Saliva contains antimicrobial proteins, immunoglobulins, and enzymes that protect gum tissue from bacterial overgrowth. When saliva production declines, gum tissue becomes more susceptible to inflammation, bacterial plaque accumulation, and early-stage gum disease (gingivitis). If unmanaged, this can progress to periodontitis, the more serious, bone-affecting form of gum disease.
Can Teeth Appear Smaller or More Worn?
Yes, in two distinct ways. Enamel erosion from acid exposure (via vomiting or dry mouth) can physically wear down tooth surfaces, making teeth appear shorter or thinner over time.
Separately, rapid facial fat loss can change the proportional relationship between the face and teeth, teeth may look more prominent in some cases, or the smile framework may appear less supported, creating an aesthetic impression of shrinkage or misalignment.
Should You Stop Using Ozempic If You Notice Changes?
No, do not stop Ozempic without consulting your prescribing physician. Dental side effects, while genuinely concerning, are manageable through a combination of improved oral hygiene, hydration, and regular dental monitoring. Stopping GLP-1 medication abruptly can have metabolic consequences. The right approach is to flag dental changes to both your dentist and your doctor so a coordinated management plan can be developed.
Does Ozempic Change Your Face and Smile Appearance?
Yes, and this is closely related to the widely discussed phenomenon known as “Ozempic Face.” Ozempic Face describes the gaunt, hollow, or prematurely aged facial appearance that can follow rapid, significant weight loss on GLP-1 medications. Fat loss is not selective, when the body sheds fat, it draws from facial fat pads as well as body stores. The result can be sunken cheeks, thinning lips, more prominent nasolabial folds, and a generally aged aesthetic that contrasts with the improved body composition the patient has worked toward.
Can Rapid Weight Loss Make Teeth Look More Prominent?
Yes. When cheek and lip volume diminish, the soft tissue framework that naturally frames the smile becomes thinner. This can make the teeth appear more exposed (particularly the upper anterior teeth) and in some cases creates a skeletal or “toothy” appearance that patients find aesthetically unsatisfying. This is not a change in the teeth themselves, but a proportional shift caused by surrounding soft tissue loss.
Does Facial Fat Loss Affect Smile Symmetry?
It can. Facial fat loss is rarely perfectly symmetrical, meaning volume may be lost more on one side than the other. This asymmetry can affect how the smile is framed, alter lip movement patterns, and change the perceived balance of the smile. For patients seeking a harmonious, well-proportioned smile, these structural changes may require cosmetic dental or facial aesthetic intervention to restore.
How Can You Prevent Dental Problems While Using Ozempic?
Prevention is significantly more effective than treatment when it comes to Ozempic-related dental changes. A structured preventive approach addresses the primary drivers such as dry mouth, acid exposure, and nutritional deficiency.
How Important Is Hydration for Oral Health?
Hydration is foundational. Adequate water intake directly supports saliva production, helps flush food debris and bacteria, and dilutes acid in the oral environment. Patients on Ozempic should aim to drink water consistently throughout the day, not just when thirsty, as the drug may blunt thirst perception. Sipping water between meals and after any episode of nausea or vomiting is particularly protective for tooth enamel.
Should You Visit a Dentist More Frequently?
Yes. Patients on GLP-1 medications like Ozempic should consider increasing dental visits from the standard twice-yearly schedule to every three to four months, at least during the initial phase of treatment. This allows for early detection of dry mouth-related decay, enamel erosion, and gum changes before they progress. Dentists can also apply professional fluoride treatments and recommend prescription-strength remineralising products.
What Oral Hygiene Routine Should You Follow?
A targeted oral hygiene routine for Ozempic users should include:
- Brush twice daily
- Use a soft-bristled brush
- Floss or use interdental brushes daily
- Use an alcohol-free mouthwash
- Apply a fluoride gel or mousse
- Wait 30–60 minutes after vomiting
- Use a saliva substitute or dry mouth spray
- Chew sugar-free gum
Consistency in these practices, combined with regular dental visits, greatly reduces the risk of Ozempic-related dental problems.
Are These Ozempic Effects on Teeth Permanent or Reversible?
The reversibility of Ozempic’s dental effects depends on how early they are identified and addressed. Dry mouth itself is reversible once the contributing factors, such as dehydration, medication side effects, are managed. Early-stage enamel erosion can be arrested and partially remineralised with fluoride and calcium phosphate treatments, though lost enamel cannot regenerate completely. Gum inflammation detected at an early stage is highly reversible with professional cleaning and improved home hygiene.
Advanced gum disease (periodontitis) and significant enamel loss, however, may require restorative or cosmetic dental treatment for full functional and aesthetic restoration. Facial volume loss from rapid weight loss is not self-reversing and may require cosmetic interventions to address.
The clear message is, addressing dental changes early significantly improves outcomes and minimizes long-term damage.
How Can Ozempic Teeth Be Treated?
Treatment depends on the type and severity of dental changes. A combination of preventive, restorative, and cosmetic approaches is most effective. Common treatment strategies include:
- Professional Cleaning: Early gum inflammation and plaque accumulation can be reversed with prophylaxis and scaling.
- Veneers or Crowns: Restore shape, length, color, and uniformity for teeth affected by enamel erosion or wear.
- Smile Design: Digital planning and holistic restoration ensure proportionality between teeth, lips, and face.
- Adjunct Cosmetic Interventions: Dermal fillers may support lip and cheek volume lost during rapid weight loss.
A comprehensive plan combining these approaches provides the best functional and aesthetic outcomes.
Can Veneers or Crowns Restore Smile Aesthetics?
Yes. For patients who have experienced visible enamel erosion, tooth wear, or aesthetic changes to their smile, porcelain veneers and dental crowns are highly effective restorative solutions. Veneers are ultra-thin porcelain shells bonded to the front surface of teeth. They restore shape, length, colour, and uniformity in a minimally invasive way. Dental crowns are used when structural damage is more extensive, providing full coverage and protection for compromised teeth. Both options can dramatically restore the appearance and confidence of a smile affected by Ozempic-related changes.
What Role Does Smile Design Play for Treating Ozempic Teeth?
Smile design (the process of digitally planning and aesthetically restoring the full smile) plays a central role in comprehensive Ozempic Teeth treatment. Because these patients often experience changes not just to individual teeth but to the overall proportional relationship between their teeth, lips, and face, a whole-smile approach is far more effective than isolated treatments.
Digital Smile Design (DSD) allows dentists to map the patient’s facial features, lip dynamics, and tooth proportions to create a result that is harmonious, age-appropriate, and flattering given their post-weight-loss facial structure.
For patients whose smile has changed significantly due to facial volume loss, smile design can be coordinated with facial aesthetic treatments (such as dermal fillers for lip and cheek support) for a fully integrated outcome.
Can Professional Cleaning Reverse Early Effects?
Professional dental cleaning (prophylaxis and scaling) is highly effective for reversing early-stage gum inflammation and removing plaque and calculus deposits that contribute to gum disease and bad breath. For patients experiencing the early signs of Ozempic-related oral changes such as gum redness, mild bleeding, increased plaque accumulation, a professional dental cleaning combined with improved home hygiene can fully resolve these early effects. It does not reverse enamel erosion, but it removes the bacterial environment that accelerates further damage, making it a critical first step in any treatment plan.
What Do Dentists Say About Ozempic Teeth?
Dentists who are seeing GLP-1 medication users in their practices report a consistent pattern: patients on Ozempic or similar medications are presenting with higher rates of dry mouth, increased cavity formation, and, in patients with rapid weight loss, notable changes to smile aesthetics. The clinical community has moved from skepticism to engagement on this topic, recognising that GLP-1 medications represent a significant enough population shift that dental practices need updated protocols for these patients.
The emerging consensus among dental professionals includes several key points: GLP-1 users need more frequent monitoring, salivary health should be assessed at every visit, and cosmetic outcomes should be discussed proactively. This is important particularly for patients undergoing significant facial changes. The dental community is also calling for better cross-specialty communication between prescribing physicians and dental providers to ensure patients receive coordinated care.
“We’re seeing more patients on GLP-1 medications presenting with dry mouth, enamel erosion, and subtle but significant changes to their smile aesthetics,” says Dt. Mumin Manassra, dentist at Vera Smile.
When Should You See a Cosmetic Dentist for Ozempic Teeth?
You should consult a cosmetic dentist if you are using Ozempic and notice any of the following:
- New or worsening tooth sensitivity that affects eating, drinking, or daily comfort
- Visible changes to tooth colour, length, or texture suggesting enamel wear
- Increased bleeding or swelling of gums that persists beyond two weeks
- Persistent dry mouth that home remedies are not resolving
- Aesthetic dissatisfaction with your smile following weight loss, particularly if your teeth appear more prominent, the smile looks asymmetrical, or facial changes have altered the appearance of your teeth
- Frequent new cavities in a patient without a prior history of significant decay
- Bad breath that does not resolve with standard oral hygiene
At Vera Smile, our team combines expertise in cosmetic and restorative dentistry with a deep understanding of how systemic health changes affect oral health and smile aesthetics. If you are concerned about the impact of Ozempic on your teeth or face, we invite you to schedule a consultation. Early assessment and personalised treatment planning can protect your oral health and ensure your smile reflects how well you feel.
Frequently Asked Questions:
Some patients report dry mouth within weeks of starting the medication. Visible enamel changes or increased cavity rates may become apparent over three to six months, particularly in high-risk individuals.
Yes. Veneers and other cosmetic treatments can be performed while you continue your medication. Your dentist will ensure your gum health is stable before proceeding with any elective cosmetic work.
Patients travelling to Turkey for dental treatments while using Ozempic should ensure their treating clinic is aware of their medication status. Clinics like Vera Smile are experienced in assessing GLP-1 users and developing treatment plans that account for the oral health dynamics of this patient group.
Stopping the medication may reduce ongoing dry mouth and acid exposure, but damage already done to enamel or gum tissue requires active dental treatment to address. It does not simply reverse on its own.